
Savonia Article: Digital transformation in health care and the role of change management
This work is licensed under CC BY-SA 4.0
What is digital transformation and how it has been implemented in our health care?
Digital transformation is a broad subject and includes multiple terms referring to the digital changes, like digital health, digitalization and digitization. Digital health solutions have become a big part of our daily lives, as wearable devices and telehealth services are used increasingly. By digitalization and digitization the information is transferred to the computer readable format, such as electronic health records. Conceptually, digital transformation differs from these related term.Digital transformation does not only include the physical change but also changes in culture and values, it is broader in scope. Digital transformation is the future of all health care related operations. (Peter, 2024 17-20; Tucker, Cirella & Kelly, 2024, 98.) The rapid development of digital technologies has transformed the health care sector, not only in Finland but also globally. By 2020, approximately 30 % of the health care services were provided through digital channels in Finland (Kyytsönen, Vehko, Jormanainen, Aalto & Mölläri, 2021). The new way of delivering care modernized the health care sector, making services more accessible and optimizing the efficiency. However, it creates a challenge for delivering equal access to care for everyone. Moreover resistance of hierarchic health care systems is a barrier for these health care improvements. (Heponiemi et. al. 2023.) To ensure that the digital transformation is adapted to the health care appropriately and used effectively and sustainable change management strategies are needed. It is crucial to understand how to manage and lead the change. Change management provides tools and strategies to guiding organizations through the change. (Pirinen 2023, Chapter 1, 3.) Recent research publications identify four key elements of change management to use for successful digital transformation in healthcare: leadership, organizational readiness, staff engagement, and strategic collaboration (Figure 1.)
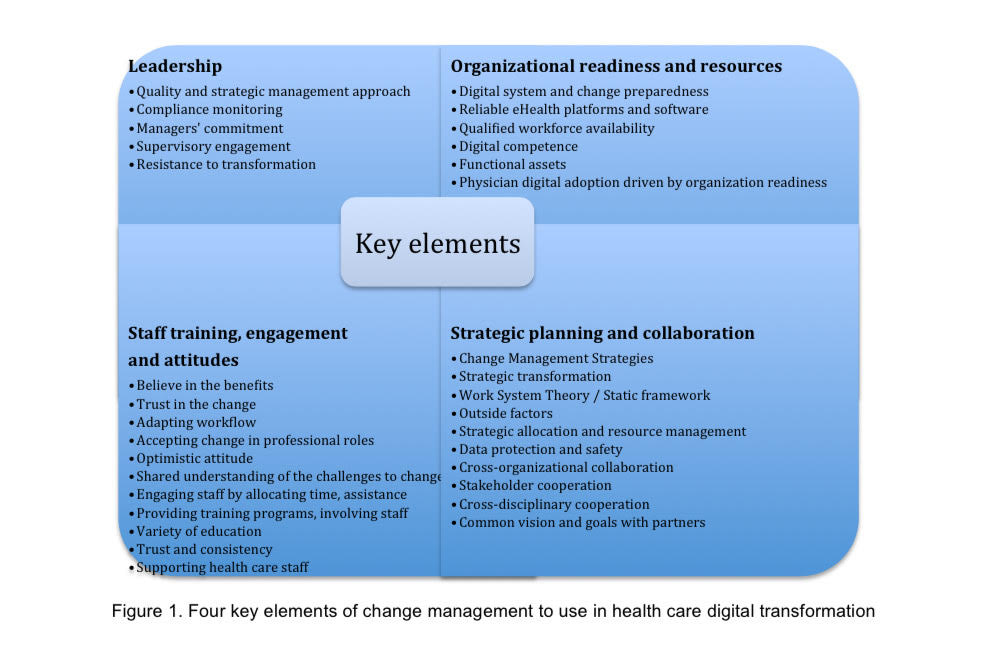
Leadership as a driver of the change
Strong leadership plays a pivotal role in navigating health care organization through digital transformation and should be applied in all management levels from senior executives to operational supervisors. By applying change management strategies and using quality and strategic point of view in organization change is proven to have positive results. (Back et. al. 2022; Bhakta, Deyhim, Zafar & Abbasi, 2022.) Management’s commitment, digital literacy and clear communication correlate directly with the success of integrating digital change and decreasing resistance to change. Supervisors are expected to engage with the change and manage allocated resources well. This way sustainable results can be enhanced. (Gustaffsson & Dannapfel 2024; Martin et. al. 2024; Brommayer, Whittaker & Liang, 2024.)
Organization readiness as a foundation of digital transformation
Digital transformation requires not just new tools, but also infrastructure to support the change. Organization needs to have proper infrastructure, financial and human resources and supportive policies to implement the change (Alshahrani, Williams & MacLure, 2022). The organization readiness can be measures with “Organizational Digital Transformation Readiness” (ODTR) framework, which guides to evaluating competence, culture, technology, and capacity before implementing the change (Michelotto & Joia, 2024). A good staff preparedness and digital competence is correlating with the success of the implementation of digital transformation (Brommayer, Whittaker & Liang, 2024; Sönling et. al. 2023). Without these preparations, even the best digital transformation may fail to be integrated to a daily operation.
Staff engagement and training as essential element in digital transformation
Health care staff must understand and accept the digital tools to ensure seamless adoption of the transformation. Positive attitudes, trust and training can reduce resistance to change (Sönling et. al. 2023; Gustafsson & Dannapfel, 2024). Variety of education should be provided and customizing the education according to the staff’s competence is important. Moreover continuous education should be provided. Involving health care staff in the transformation for early on is recommended. (Back et. al.2022; Bhakta et. al. 2022.) Health care staff needs support during the transition to adopt new ways of working (Martin et. al. 2024; Petersson et. al. 2024; Naamati-Schneider, Arazi-Faldon & Daphna-Tekoah, 2025).
Strategic planning and collaboration as the framework holding change together
Digital transformation has to be well planned and using change management strategies enables the planning (Bhakta et. al. 2022; Jewer, 2022). Laws and regulations for the health care sets certain frameworks they should be considered when planning the change (Petersson et. al. 2022). Managing the strategy and resources with making sure organization policies are followed requires detailed planning. Digital data has to be well protected and it affects on health managers ideas of digital transformation. (Brommayers, Whittaker & Liang, 2024; Alshahrani, Williams & MackLure, 2022.) Working together with other organizations can bring benefits. The barriers between different departments and organizations should be minimized (Brommayer, Whittaker & Liang 2024; Alshahrani, Williams & MacLure, 2022; Sibuyi, de la Harpe & Nyasulu, 2022; Bhakta et. al. 2022.) Having a common goal and vision; and stakeholder collaboration creates a positive base for sustainable digital transformation in health care (Gustafsson & Dannapfel, 2024).
Conclusion
Health care’s digital transformation is worldwide present-day process. This article shows that technological change alone is not enough. Effective change management, concentrating on leadership, organizational readiness, staff empowerment, and strategic planning and collaboration are essential for sustainable success. By concentrating on these key areas, health care systems can ensure that digital transformation lead not only to greater efficiency but also to better care for all.
Author:
Jonna Mäki-Koivisto, Master’s Degree in Digital Health, Savonia University of Applied Sciences
References:
Alshahrani, A., Williams, H., Maclure, K. 2022. Investigating Health Managers’ Perspectives of Factors Influencing Their Acceptance of eHealth Services in the Kingdom of Saudi Arabia: A Quantitative Study. Saudi Journal of Health Systems Research, [s. l.], v. 2, n. 3, p. 114–127, 2022. Available: https://research.ebsco.com/linkprocessor/plink?id=929ab69c-6768-3fbf-9b13-574b966c5fb8. Accessed: 3.3.2025.
Back, D.A., Estel, K., Pförringer, D., Tsitsilonis, S., Bachner, J., Willy, C., working group digitalization (DGOU) & Becker H. P. 2022. Implementation of online video consultations in a regional health network: a management feasibility analysis from an orthopedic perspective. BMC Health Services Research, [s. l.], v. 22, n. 1, p. 1–11, 2022. Available: https://research.ebsco.com/linkprocessor/plink?id=9cdee4c1-cc92-3ca1-8080-bed6a35f2363. Accessed: 3.3.2025.
Bhakta, S. B., Deyhim, N., Zafar, N. & Abbasi G. A. 2022. Implementation and evaluation of an EHR-intergated mobile dispense tracking technology in a large academic tertiary hospital. American Journal of Health-System Pharmacy, [s. l.], v. 79, n. 18, p. 1562–1569, 2022. Available: https://research.ebsco.com/linkprocessor/plink?id=38b94462-fadd-3bc4-bb3b-366e322fcd44. Accessed: 3.3.2025.
Brommeyer, M., Liang, Z., Whittaker, M. & Mackay M. 2023. Developing Health Management Competency for Digital Health Transformation: Protocol for a Qualitative Study. Available: https://www.researchgate.net/publication/374717662_Developing_Health_Management_Competency_for_Digital_Health_Transformation_Protocol_for_a_Qualitative_Study. JMIR Res Proto 12:e51884. Accessed: 6.12.2024.
Gustafsson, C. & Dannapfel, P. 2025. Leaders’ experiences of successfully implementing health and welfare technology in sparsely populated Nordic areas. Disability & Rehabilitation: Assistive Technology, [s. l.], v. 20, n. 1, p. 85–96, 2025. DOI 10.1080/17483107.2024.2352130. Available: https://research.ebsco.com/linkprocessor/plink?id=e3b7577f-3ca7-3e7f-ac81-bdafdbb1105b. Accessed: 3.3.2025.
Heponiemi, T., Kainiemi, E., Virtanen, L., Saukkonen, P., Sainio, P., Koponen, P., Koskinen, S. 2023. Predicting Internet Use and Digital Competence Among Older Adults Using Performance Test of Visual, Physical and Cognitive Functioning: Longtudinal Population-Based Study. J Med Internet Res. 2023 May 5;25. Available: https://pmc.ncbi.nlm.nih.gov/articles/PMC10199390/. Accessed: 4.12.2024.
Jewer, J. 2022. Investigating a Work System Approach to Implement an Emergency Department Surge Management System: Case Study. Journal of Medical Internet Research, [s. l.], v. 24, n. 8, p. N.PAG, 2022. Available: https://research.ebsco.com/linkprocessor/plink?id=bccfec53-49b0-3551-ae25-fb5dca0b5247. Accessed: 3.3.2025.
Kyytsönen, M., Vehko, T., Jormanainen V., Allto A-M., Mölläri, K. 2021. Terveydenhuollon etäasioinnin trendit vuosien 2013-2020 Avohilmon aineistossa. Finnish Institute for Health and Welfare. Available: https://urn.fi/URN:ISBN:978-952-343-639-8. Accessed: 4.12.2024.
Martin, T., Veldeman, S., Großmann, H., Fuchs-Frohnhofen, P. Czaplik, M. & Follmann, A. 2024. Long-Term Adoption of Televisits in Nursing Homes During the COVID-19 Crisis and Following Up Into the Postpandemic Setting: Mixed Methods Study. JMIR Aging. 2024 Jun 6;7:e55471.
Michelotto F. & Joia, L. A. 2024. Organizational Digital Transformation Readiness: An Exporatory Investigation. J. Theor. Appl. Electron. Commer. Res. 2024, 19(4), 3283-3304. Available: https://www.mdpi.com/0718-1876/19/4/159. Accessed: 12.4.2025.
Naamati-Schneider, L., Arazi-Fadlon, M., Daphna-Tekoah, S. 2025. Strategic technological processes in hospitals: Conflicts and personal experiences of healthcare teams. Nursing Ethics. 2025;32(1):236-252. [s. l.], v. 32, n. 1, p. 236–252, 2025. Available: https://research.ebsco.com/linkprocessor/plink?id=5fbfa24a-42bd-3e52-9499-420f531b6754. Accessed: 3.3.2025.
Peter, M.K. 2024. The Digital Transformation Canvas; Develop and implement your digital strategy. Pearson Education Limited: Harlow, United Kingdom.
Petersson, L., Larsson, I., Nygren, J. M., Nilsen, P., Neher, M., Reed, J. E. Tyskbo, D., & Svedberg, P. 2022. Challenges to implementing artificial intelligence in healthcare: a qualitative interview study with healthcare leaders in Sweden. BMC health services research, 22(1), 850. Available: https://doi.org/10.1186/s12913-022-08215-8. Accessed: 3.3.2025.
Pirinen, H. 2023. Esihenkilö muutoksen johtajana. Helsinki: Alma talent. Available: https://savonia.finna.fi/Record/savonia.994908005306248?sid=4882753650. Accessed: 9.12.2024.
Sibuyi, I. N., de la Harpe, R. & Nyasulu, P. 2022. A Stakeholder-Centered mHealth Implementation Inquiry Within the Digital Health Innovation Ecosystem in South Africa: MomConnect as a Demonstration Case. JMIR mHealth and uHealth, 10(6), e18188. Available: https://doi.org/10.2196/18188. Accessed: 3.3.2025.
Söling, S., Demirer, I., Köperlein-Neu, J., Hower, K. I., Müller, B. S., Pfaff, H., Karbach U. & AdAM Study Group. 2023. Complex implementation mechanisms in primary care: do physicians’ belief about the effectiveness of innovation play a mediating role? Applying a realist inquiry and structural equation modeling approach in a formative evaluation study. BMC Primary Care, s. l.], v. 24, n. 1, p. 1–14, 2023. Available: https://research.ebsco.com/linkprocessor/plink?id=df2b0c43-0e7c-349d-b594-7c770a141277. Accessed: 3.3.2025.
Tucker, D.A., Cirella S. & Kelly, P.R. 2024. Organizational change management: inclusion, collaboration and digital change in practice. Sage: London.